There are two types of primary knee replacement surgery – total knee replacement and partial knee replacement. Mr Tarique Parwez, Consultant in Trauma & Orthopaedic Surgery answers some commonly asked questions to explain the difference between the two procedures, when surgery would be advised and how long it will take to resume normal activities after surgery.
When is a total or partial knee replacement usually recommended?
When all non-operative measures to manage and treat knee arthritis have been tried and pain is interfering with quality of life, a total or partial knee replacement is often recommended.
What are non-operative measures?
Non-operative treatments include lifestyle changes and modification of activities, weight loss, walking aids, braces, anti-inflammatory pain relief and physiotherapy.
Why do I have to suffer so long before being offered a knee replacement?
Knee replacement is an excellent option when other measures have failed but a natural knee is a complex structure. Every individual knee is a different shape and size. Artificial knees come in a limited range of sizes so it can be difficult to replicate the exact geometric shape needed. As a result, some of the knee mechanism is altered or removed to perform the surgery. This leads to some residual discomfort and the feeling that it’s not a natural knee. It’s also cemented to the bone and, while modern techniques are more robust, the fixing can loosen after sometime (15-20 years). Therefore, your consultant will always want to make sure all other options have been tried before replacing the natural knee with an artificial one.
 What is total knee replacement?
What is total knee replacement?
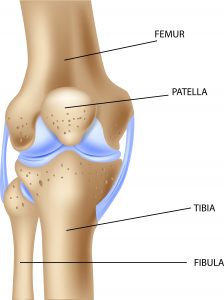
Total knee replacement is the most common type of knee replacement, particularly for ages 60 – 80. The knee joint is made up of the lower thigh bone (femur), the upper shin bone (tibia) and the knee cap (patella). Normally the knee allows the thigh and shin bone to slide over each other due to the smooth cartilage which covers them and lines the underside of the kneecap. When cartilage is worn away through wear and tear, injury or arthritis, the joint becomes stiff and can cause pain. A total knee replacement replaces the surfaces of both the thigh bone and shin bone that connect to the knee.
What is knee replacement prosthesis made of?
My preference is to use a prosthesis where the thigh bone component is stainless steel, the shin bone tray is titanium and there is a plastic sandwich in between (UHMWPE).
What is partial knee replacement?
In most cases osteoarthritis begins in the front inside part of the knee and gradually other parts get worn out due to abnormal motion. If identified in time just replacing the worn out part, usually the inside half of the knee, can slow down or halt the process of complete wear out of the knee.
What are the advantages and disadvantages of a partial replacement?
As the two thirds of the natural knee remains in place and ligaments are not removed, the partially replaced knee moves and behaves more like a natural knee allowing individuals to lead a more active lifestyle, for example climbing, walking on uneven grounds. Some partial knee replacements are performed without the need of cement so there is no risk of loosening as a cause of failure. A partial knee replacement is more suited to young active individuals with heavier demand on their knees. The disadvantages are that the procedure is technically more demanding and can lead to early failure due to surgical technique. Also, because it’s easier to revise than a total knee replacement the knee will sometimes get revised due to residual pain which most artificial knees will have whether partial or total. Although with partial knee replacement there is less residual pain.
How successful is knee replacement?
According to Patient Reported Outcome measures, 90-95% patients are satisfied or very happy with the result. Is it better than 0%? Definitely Yes! Is there guaranteed 100% pain relief? No.
A knee replacement, total or partial, will allow an individual to walk unlimited distances, enjoy their hobbies and play doubles tennis but anything more vigorous is not encouraged as it might lead to early loosening of the prosthesis.
How long does it last?
According to the 16th National Joint Report only 96.5% of common established brand knee replacements performed 15 years ago are still working. We expect that with contemporary techniques and an increase in our knowledge of what causes a failure, knee replacement today will still be working in 15-20 years in most individuals. Contemporary partial knee replacements have 93% survival at 10 years. Newer implants are showing even better promising result. It is hoped that it would last as long as a total knee replacement and with life expectancy increasing one might only need revising to a simple total knee prosthesis rather than a complex revision prosthesis in their lifetime.
What are the risks of knee replacement surgery?
No procedure is without risks. Common risks are DVT, infection (less than 0.5%), wound issues, stiffness, residual discomfort, and swelling.
What are the latest techniques in knee replacement surgery?
Improvements are being made all the time to improve techniques and the longevity of the replacement. Computer assisted, or navigated surgery improves the accuracy of desired component placement and is essential in certain cases where there is major deformity or prior injury to the limb. Robotic knee surgery also improve accuracy of the implant placement. Customized knee replacements and patient specific instrumentation are individualised to a patient’s knee. This technique is not without its challenges as there is little leeway if the sizing needed is slightly different. It needs to be seen if it leads to higher satisfaction and longevity. Patient specific Instrumentation similarly aims to improve accuracy by having specific cutting jigs/blocks for doing the surgery made specifically for an individual.
What is the recovery time for total knee replacement surgery?
Everyone heals from total knee replacement surgery at a different pace. In most cases, however, you will likely use a walker or crutches for 2 to 4 weeks after your operation. You will then advance to a cane and wean to no assistive device at all. You will gradually return to normal function without any assistive devices. In general, most patients are close to full recovery after 3 months. With partial knee replacement the recovery time is much quicker.
Will I need physiotherapy afterwards?
Yes. You will see a physiotherapist while in hospital and will remain in their care after your operation and they will guide you through the rehabilitation exercised.
When do my stitches or staples come out after knee replacement surgery?
Your surgeon may close your wound in a variety of ways. If you have staples, they should be removed 2 weeks post-operatively. If you have stitches that are absorbed they do not need to be removed. Some wounds have a tail of suture that is visible at each end of the incision. You may trim this level with the skin at 2 weeks.
When do I need to follow-up with my surgeon?
Follow-up appointment should be made post-operatively at 72hrs with the physiotherapist, and 6 weeks with your surgeon . Additional follow-ups will be scheduled as required.
When can I shower after total knee replacement surgery?
You may shower (get the incision wet) three days after your operation. If no drainage is present at the incision, no protection of the wound is required. If there is drainage from the incision, try to keep it covered and dry while showering.
When can I immerse my knee in water after knee replacement surgery?
You may immerse your knee in water (e.g. bath, swimming pool, hot tub) after three weeks if there is no drainage from the incision. The incision must be healed before it is immersed in water.
How long will I be on pain medication after knee replacement surgery?
You will likely require some form of pain medication after your hospital stay. Initially, you will be on a strong oral pain medication. Most people are able to wean off of their strong pain medication after 1 month and are able to switch to an over-the-counter/simpler painkiller. If you are on blood thinners, avoid taking any anti-inflammatory drugs without first consulting your doctor.
Should I use ice or heat after total knee replacement surgery?
Ice can be used for the first few weeks especially after doing your physiotherapy exercises , or if you have a lot of swelling or discomfort. Once the initial swelling has decreased, you may use ice and/or heat.
Should I wear compression stockings (TEDS) after total knee replacement surgery?
Compression stockings are not required post-operatively after discharge from the hospital. In the past it was prescribed for six weeks but incorrect usage causes more harm.
What are good positions for my knee? What positions should I avoid?
You should spend some time each day working on straightening your knee (extension) as well as bending your knee (flexion). A good way to work on extension is to place a towel roll underneath your ankle when you are lying down. A good way to work on flexion is to sit on a chair or stationary bicycle and bend your knee. Avoid using a pillow or towel roll behind the knee for any length of time.
Can I use weights after knee replacement surgery?
Generally, you should not use weights for the first two months after knee replacement surgery. However, as everyone’s strength varies, consult with your physiotherapist before using weights. Use light weights to begin with and gradually progress. Avoid exercises that cause significant discomfort or pain.
When can I drive after total knee replacement surgery?
If you had surgery on your right knee, you should not drive for at least six weeks. After six weeks you may return to driving if you feel comfortable and can do an emergency stop with ease. If you had surgery on your left knee, you may return to driving when you feel comfortable as long as you have an automatic transmission. Do not drive if you are taking strong pain medication. Most importantly, do not take chances, and only resume driving if you are confident in yourself. It is recommended that you test your driving ability prior to driving in traffic.
When can I return to work after knee replacement surgery?
When you can return to work depends on your profession. If your work is desk based you may return as early as 2 to 4 weeks post-operatively. If your work is more rigorous, you may require up to 3 months before you can return to full duty. In some cases, more time may be necessary.
What activities are permitted following knee replacement surgery?
You may return to most activities as tolerated, including walking, gardening, and golf. Some of the best activities to help with motion and strengthening are swimming and a stationary bicycle.
What activities should I avoid after knee replacement surgery?
You should avoid high impact activities, such as running and vigorous racquet sports, such as singles tennis or squash.
Can I drink alcohol after total knee replacement surgery?
If you are on blood thinners, avoid alcohol intake. Otherwise, use in moderation at your own discretion. You should also avoid alcohol if you are taking strong pain medication.
When can I fly to go on holiday?
If you’re progressing satisfactorily and there are no wound issues you may take a short haul flight after six weeks but for long haul flights it’s advisable after twelve weeks and even then you have to take adequate extra precaution on the flight like keeping yourself well hydrated, doing static calf exercises and taking a few walks around the aisles if safe.
Can I kneel after total knee replacement surgery?
After 2 months, you may try to kneel. Although this may be uncomfortable initially, you will not injure your knee replacement by kneeling. Most people find the more you kneel, the easier it gets.
Can I go up and down stairs after total knee replacement surgery?
Yes. Initially, you will lead with your non-operated leg when going up stairs and lead with your operated leg when going down stairs. You can use the phrase, “Up with the good, down with bad” to help you remember. As your leg gets stronger (after about 1 month), you will be able to perform on stairs in a more regular pattern.
Will my leg get straighter after surgery?
Yes. That’s one of the main aims of surgery
I think my leg feels longer after total knee replacement surgery. Is this possible?
In the large majority of cases, leg length is essentially unchanged after total knee replacement surgery. In rare cases, however, you may notice a change in leg length. This is more common when a severe deformity of the knee exists before surgery. At first, this may feel awkward. However, you will gradually become accustomed to your new knee and leg length.
I feel depressed after total knee replacement surgery. Is this normal?
It is not uncommon to have feelings of depression after your knee replacement. This may be due to a variety of factors, such as limited mobility, discomfort, increased dependency on others, and/or medication side effects. Feelings of depression will typically fade as you begin to return to your regular activities. If your feelings of depression persist, consult your GP.
I have insomnia after total knee replacement surgery. Is this normal? t it?
Insomnia is a common complaint following total knee replacement surgery. Non-prescription remedies may be effective. If insomnia continues to be a problem, medication may be prescribed for you by your GP.
If I am concerned about my new knee, what should I do?
As I guide, below is a list of what is normal and when you should seek medical advice.
Normal things about your new knee.
- Clicking noise with knee motion
- Skin numbness on the outer (lateral) part of your knee
- Swelling around knee and/or lower leg
- Warmth around knee
- Pins and needles sensation at, or near, incision
- Dark or red incision line. This will gradually fade to a lighter colour.
- Bumps under the skin along the incision. Occasionally, the sutures used to close the wound can be felt
- Bruising
Abnormal things about your new knee. Seek medical advice immediately if you experience any of these.
- Increasing redness, particularly spreading from incision
- Increasing pain and swelling
- Fever (>38 C)
- Persistent drainage from your wound
- Calf swelling or pain, particularly associated with ankle motion
- Ankle swelling that does not decrease or resolve overnight
- Bleeding gums or blood in urine/stool



 One Ashford
One Ashford One Hatfield
One Hatfield