Every year, several conventional total shoulder replacements are successfully performed in the UK for patients with shoulder arthritis. This type of surgery, however, is less beneficial for patients with large rotator cuff tears who have developed a complex type of shoulder arthritis called “cuff tear arthropathy.” For these patients, a conventional total shoulder replacement may result in persistent pain and limited motion, and a reverse total shoulder replacement is a better option.

A conventional shoulder replacement device mimics the normal anatomy of the shoulder: a plastic “cup” is fitted into the shoulder socket (glenoid), and a metal “ball” is attached to the top of the upper arm bone (humerus). In a healthy shoulder, the rotator cuff muscles help position and power the arm during range of motion. A conventional replacement device also uses the rotator cuff muscles to function properly.
In a patient with a large rotator cuff tear and cuff tear arthropathy, these muscles no longer function adequately. The reverse total shoulder replacement relies on the deltoid muscle, instead of the rotator cuff, to power and position the arm. In a reverse total shoulder replacement, the socket and metal ball are switched. The metal ball is fixed to the socket and the plastic cup is fixed to the upper end of the humerus. The reverse total shoulder replacement works better for people with cuff tear arthropathy because it relies on a separate set of intact muscle (the Deltoid) to move the arm.
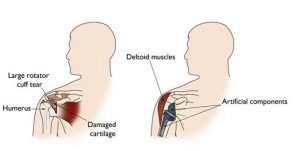
(Left) Rotator cuff arthropathy.
(Right) The reverse total shoulder replacement allows other muscles – such as the deltoid – to do the work of the damaged rotator cuff tendons.
Candidates for Surgery
Reverse total shoulder replacement may be recommended if you have:
- A completely torn rotator cuff that cannot be repaired reliably
- Arthritis associated with a rotator cuff tear
- A previous shoulder replacement that was unsuccessful
- Severe shoulder pain and difficulty lifting your arm away from your side or over your head
- A complex fracture of the shoulder joint
- A long-standing unreduced shoulder dislocation
- A tumour of the joint
- Failure to respond to other treatments, such as rest, medications, cortisone injections and physical therapy that have not relieved shoulder pain.
They may have marked limitation in the function affecting even simple tasks of daily living such as taking care of their own hygiene, feeding themselves, getting dressed and undressed. This lack of function can make the difference between a person being independent or needing 24/7 nursing.
Reversed shoulder prostheses are gaining popularity in recent years. Good mid-term results with restoration of active elevation have been reported.
However there is a high complication rate with stemmed prostheses ranging between 24% – 50% in different series and many of them require further surgery.
Of major concerns are glenoid (socket) or humeral shaft fractures (arm bone) on preparation, dislocations and instability as well as high infection rate. Glenoid notching is a serious complication that was noticed in over 70% of cases with Grammont type of prosthesis and seems to appear quite early at 2 – 3 months post operatively (Levigne et al., J Shoulder Elbow Surg 2008). The amount of bone resected for the insertion of stemmed prosthesis make any further revision surgery very difficult and therefore the use is limited to the very elderly patients.
The Verso Stemless Reverse Total Shoulder Replacement System is a novel design bone preserving reverse geometry prosthesis. This prosthesis has been developed for use in rotator cuff deficient shoulders with arthritis following extensive research since 1997 and it has been in clinical use for 12 years. The rationale behind the design of the Verso was to create a simple yet sophisticated implant. When the implant and technique are simple, there are fewer places for errors. Some of the important differences between the Verso and other available reverse shoulder replacements are as follows:
Minimal bone resection
This limits the amount of native bone compromised. Only about 20mm of bone is resected. The resected bone is recycled into the remaining bone and used for bone impaction to improve the quality of early fixation of the implant in the patient.
Stemless, cementless fixation
There are only 3 thin fins which, combined with bone impaction technique gives immediate press fit fixation of the prosthesis to the upper end of the arm bone (humerus) and further biological fixation from the porous and hydroxyapatite coating. This design provides direct load transfer to the humeral metaphysis, which greatly reduces stress shielding, and proximal bone absorption and preserves the quality of the bone.
Improved rotational movements
By a specially designed plastic cup, that reduces impingement and the serious problem of notching.
All options remain open for future surgery if deemed necessary as bone stock is preserved.
Reverse Shoulder Replacement surgery is available at One Ashford Hospital with Mr Jai Relwani. Initial consultations are available with short waiting times.
One Ashford Hospital is well placed to see patients from Ashford, Canterbury, Maidstone, Dover, Folkestone and all surrounding areas. To book an appointment, call the hospital direct on 01233 364 022 or email here.
Why Choose One Ashford Hospital
• Access to leading Consultants within 48 hours*
• 0% and low interest finance options**
• Competitive fixed-price packages
• Modern purpose-built hospital
• Fast access to diagnostics including MRI, X-ray and Ultrasound
• Private, spacious, en-suite rooms
• Specialist Physiotherapy and nursing teams
• Little waiting time for surgery
• Calm, dignified experience
*Dependent on Consultant availability
**Terms and conditions apply
COVID-19
The safety of our patients is of the utmost important to us. To learn more on the safety guidelines One Ashford Hospital has implemented during the COVID-19 pandemic, please click here

 One Ashford
One Ashford One Hatfield
One Hatfield